Real-World Cases Cited in Lecture on Dermoscopy Use Beyond Pigmented and Nonpigmented Lesion Examination
Various sessions during SDPA Annual Summer Conference 2021 covered general and niche uses for dermoscopy, concluding that the dermatoscope is a valuable, clinically significant tool—as long as you have it with you! Roman Bronfenbrener, MD (pictured, right), from Penn Derm Specialists and University of Pennsylvania in Philadelphia, Pennsylvania, began his session “Dermoscopy: Clinical Uses Beyond Pigmented Lesions,” by stating that dermoscopy has utility in the diagnosis and management of multiple general dermatologic cases outside of pigmented and nonpigmented lesion examination. Dermoscopic applications have been described for psoriasis, eczema, rosacea/acne, and alopecia as well as bacterial, viral, parasitic, and fungal infections; and other granulomatous diseases, such as foreign body reactions. However, as Dr. Bronfenbrener, points out, implementing dermoscopy into clinical practice requires one important first step—making sure your dermatoscope is accessible for use rather than for example in your bag or desk drawer. “You can’t use it if you don’t have it!” he said, segueing into a discussion on how to acquire the best image.
SPECIAL COVERAGE: SDPA Annual Summer Conference 2021, Chicago, July 22-25, 2021
In lesional dermoscopy, you usually want a medium like rubbing alcohol or sanitizer between the dermatoscope and the skin. When looking at general dermatology conditions under dermoscopy, scale is important, meaning that the clinician should take an initial “dry” dermoscopic view without any mediums applied. Remembering to practice “dry dermoscopy” can be crucial in getting the best image to aid in diagnosing conditions. For example, when looking for lichen planopilaris (LPP), applying a medium like alcohol to the skin can cause perifollicular scale, a key diagnostic clue of LPP, to disappear. Another consideration in utilizing dermoscopy in clinic is visualization of vascular structures, an important aspect of both lesional and general dermoscopy, but even more so in general cases. Dr. Bronfenbrener cautions that care should be taken not to press too hard against the skin with the dermatoscope as doing so could “blanche out” visual on vascular and other structures needed to make a diagnosis. He also encouraged clinicians to take pictures of individual areas so they can go back and learn from them once the final diagnosis is in hand. “Some features are only apparent in hindsight,” he said. “It’s easy to do, and you’ll become a better provider for it,” he concluded.
Next, Dr. Bronfenbrener presented a series of real-world patient cases to illustrate how dermoscopy assists in various general dermatology conditions. Case presentations followed a grand rounds format, showing clinical images, giving a brief patient presentation, and prompting attendees to ponder then select the best course of action among multiple choices. Cases demonstrated exactly how dermoscopy aided in ultimate diagnoses, which were shown to be further supported by findings in the literature. The following lists highlights from the cases presented.
Case Presentation. A 49-year-old man presents with a rash of four weeks duration (see picture below). The rash is asymptomatic at time of presentation, but the patient reported it was itchy prior to this current visit. His medical history revealed that he was on no medications and was otherwise healthy. Of note, he started exercising at the gym six weeks prior to presentation and mentioned he was “sweating a lot” in this area. He also had a history of toenail fungus, which had been previously treated with efinaconazole. Given only the naked-eye image of the patient’s skin rash, the attendees voted on probable diagnosis from the following options: a) erythema annulare centrifigum, b) tinea cruris/tinea corporis, c) pigmented purpura, d) sarcoidosis, e) cutaneous T-cell lymphoma (CTCL), f) secondary syphilis, g) erythema chronicum migrans, h) necrobiosis lipoidica, or i) all of the above.
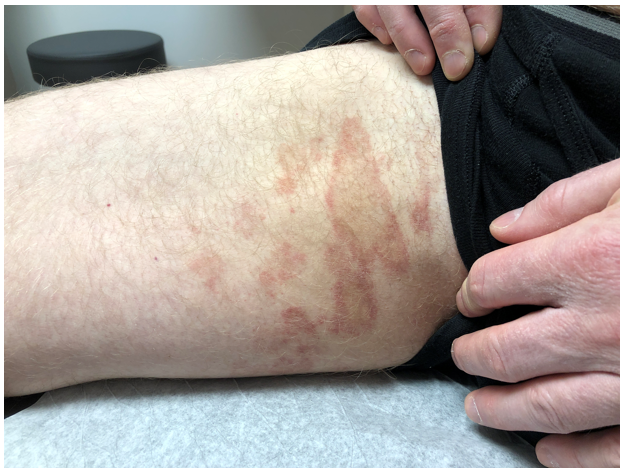
See Case Presentation Description Above
“We are going all the way out into Neverland as far as the diagnoses go, but all of these are uncommon and could look like this,” Dr. Bronfenbrener said.
Dermoscopic imaging showed purpuric globules and orange-brown background pigment with brown “flakes.” Biopsy revealed that the areas of purpuric globules correlated with a hemorrhage in the papillary dermis and the brown flakes or “peppering” correlated with melanophages in the dermis, consistent with diagnosis of pigmented purpura dermatosis (PPD).
“It’s an unusual diagnosis and not something that walks into the clinic every day and dermoscopy might help you head in the right direction [of diagnosis],” Dr. Bronfenbrener said.
Key takeaway tips from this case:
- Biopsy where you are likely to find diagnostic features (e.g., within areas of purpuric globules and dots).
- You can predict subtype of PPD based on clinical, but also dermoscopic appearance.
- CTCL is in the differential diagnosis (DDx) for pigmented purpuric eruptions. Dermoscopy is still of questionable utility to differentiate between CTCL with PPD phenotype, and unusual presentations deserve close follow up and appropriate work-up.
- PPD features should not change with pressure.
- PPD can be distinguished from some clinical mimics with dermoscopy.
In conclusion, dermoscopy has many uses within a busy general dermatology clinic. It is useful to find prime biopsy location for dermatoses such as PPD, diagnose various common forms of alopecia, identify differences between common infections and infestations of the skin, and diagnose and treat foreign body implantation.
Byline: Angela Saba, Managing Editor, Journal of Dermatology for Physician Assistants
Pictured: Roman Bronfenbrener, MD, delivering a presentation during the SDPA Annual Summer Conference 2021 in Chicago (July 22-25, 2021).
Posted: August 13, 2021
